The World Health Organization (WHO) reports that 1 in 10 patients is harmed during healthcare delivery. More than 3 million deaths worldwide happen due to unsafe care. Even more concerning, over half of that harm is preventable with better systems, safer processes, and stronger oversight.
That’s not a small problem. It’s a crisis. And it’s exactly why risk management in healthcare matters.
Healthcare risk management is a process that identifies, assesses, and controls threats to a healthcare organization’s patients, staff, data, and operations. These risks fall into five broad categories:
- Clinical
- Operational
- Financial
- Legal/regulatory
- Technology
It’s not optional, either. Effective risk management is both a patient safety imperative and a regulatory requirement under HIPAA and similar frameworks.
In this guide, you’ll learn what healthcare risk management looks like in practice. We will:
- Break down the five main types of risk
- Explain the risk management process step by step
- Outline the key frameworks that shape compliance
- Discuss who is responsible
- Highlight best practices that healthcare organizations can use to build a stronger risk culture
Highlights
- Five risk areas. Healthcare risk management focuses on five main risks. These include clinical, operational, financial, legal, and technology risks.
- Patient safety. Good risk management helps prevent medical errors and patient harm. It also protects healthcare organizations from costly incidents.
- Risk management process. The process follows a clear cycle. First, identify risks. Then assess, reduce, and monitor them over time.
- Enterprise risk management (ERM). ERM helps organizations manage risks across departments. It gives leaders a clearer view of clinical, financial, legal, and cybersecurity risks.
- Strong risk programs. Healthcare organizations run regular risk assessments. They manage vendor risks, train staff, and use risk management software to track issues.
Why Is Risk Management Important in Healthcare?
In healthcare, risk management touches every part of how a healthcare organization operates. From the exam room to the server room. Here’s why it matters.
- Financial protection. Unmitigated risks add up quickly. Malpractice claims, regulatory fines, and operational disruptions all carry real costs. For example, the global average cost of a data breach is $4.4 million (Source: IBM).
- Organizational reputation. One high-profile incident can permanently damage patient trust. This can include a data breach, surgical error, or compliance failure. Reputations take years to build and days to lose.
- Regulatory compliance. Healthcare organizations must comply with HIPAA, CMS Conditions of Participation, OSHA, and numerous state laws. Risk management keeps those requirements consistently met and documented.
- Value opportunity. Risk management isn’t only about preventing losses. It also helps organizations identify and capture value opportunities that might otherwise be missed.
- Accreditation and licensing. Accrediting bodies like The Joint Commission require documented risk management programs as a condition of accreditation.
- Patient safety. Proactively identifying and mitigating clinical risks reduces adverse events, medical errors, and preventable harm.
What Are the Types of Risk in Healthcare?
Healthcare organizations face many types of risk. These can affect patient safety, operations, finances, compliance, and technology systems.
1. Clinical / Patient Safety Risk
This is the most direct type. It includes:
- Hospital-acquired infections
- Surgical complications
- Medication errors
- Misdiagnosis
What governs these risks are clinical protocols, accreditation standards, and medical licensing requirements. When something goes wrong here, patients get hurt.
2. Operational Risk
Day-to-day operations carry a real risk of disrupting care. These can include:
- Equipment malfunctions
- Supply chain failures
- Staffing shortages
- Facility hazards
Physical environment risks, such as fire codes and ADA compliance, fall under this as well. So does business continuity planning.
3. Financial Risk
Financial risks can arise from several factors, including:
- Revenue cycle vulnerabilities
- Malpractice litigation costs
- Reimbursement disputes
- Insurance gaps
Left unmanaged, clinical and operational risks can quickly turn into budget overruns. They can also lead to unexpected capital expenses.
4. Legal / Regulatory Risk
Healthcare organizations must follow a complex set of regulatory requirements. Common legal and regulatory risks include:
- Non-compliance with state privacy and health regulations
- Violations of HIPAA privacy and security rules
- Failure to meet CMS participation conditions
- OSHA workplace safety violations
Managing these requirements in isolated silos often leads to duplicated work and compliance gaps.
An enterprise risk management approach helps organizations identify overlapping requirements. This can include fire prevention standards shared across CMS, OSHA, and local fire codes. It addresses them through coordinated policies and processes.
This domain also covers documentation requirements and audit preparedness. There’s also the real risk of enforcement action.
5. Technology / Cybersecurity Risk
This covers:
- Connected medical devices
- Third-party vendor access
- Software vulnerabilities
- Network infrastructure
- Data security
Take the 2024 Change Healthcare ransomware attack. It exposed data for over 190 million individuals, according to the American Hospital Association. A reminder of what’s at risk.
Bank of America reports that 41% of healthcare data breaches originate from third parties. This is the highest rate of any industry.
And the problem isn’t improving. The HIPAA Journal reveals that 68% of covered entities and 79% of business associates find their current vendor risk management processes inefficient.
The HIPAA Security Rule requires a formal risk assessment of all threats to electronic protected health information (ePHI).
How Does the Healthcare Risk Management Process Work?
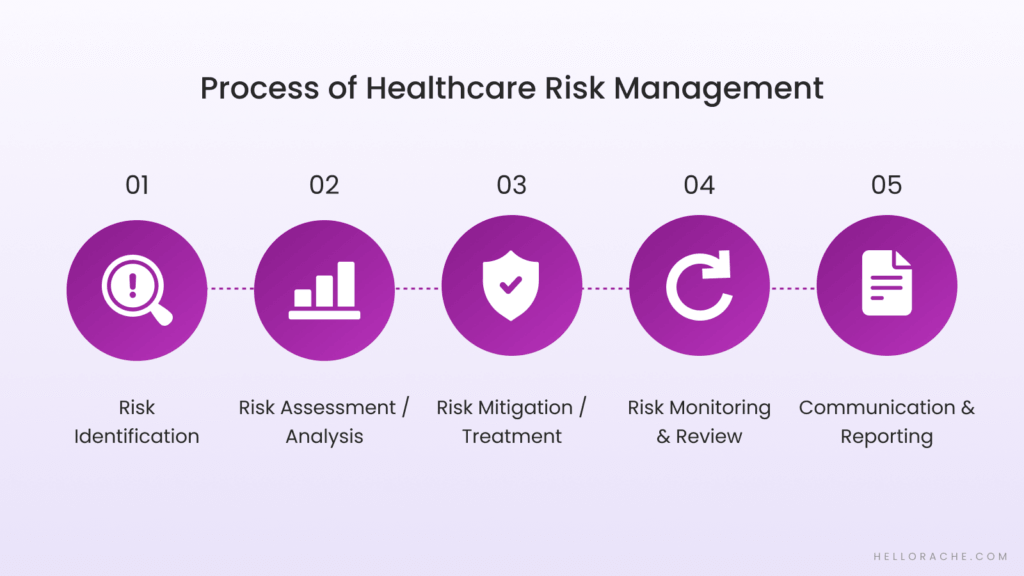
Healthcare risk management is an ongoing cycle. Here’s how it works, step by step.
Step 1: Risk Identification
The first step is systematically identifying risks across all five domains. We’ve already discussed these. They include clinical, operational, financial, legal/regulatory, and technology.
These are the risk identification methods:
- Technology vulnerability scans
- Incident reporting systems
- Patient complaint analysis
- Workflow reviews
- Staff interviews
- Audits
For HIPAA compliance, organizations must also conduct a formal security risk assessment (SRA). It helps identify all risks to electronic protected health information (ePHI).
Step 2: Risk Assessment / Analysis
Once you identify the risks, you have to evaluate them. That means looking at two things:
- How likely it is to occur
- How severe the impact would be
From there, you assign a risk score. You can classify scores as low, medium, or high. Another option is to use a numerical risk matrix to prioritize response.
Document everything. HIPAA requires risk assessment documentation to be retained for at least six years.
Step 3: Risk Mitigation / Treatment
For each identified risk, choose a response strategy: Avoid, Reduce, Transfer, or Accept.
From there, develop and implement a remediation plan. Assign clear owners, set timelines, and set up risk control measures.
For HIPAA-regulated risks, that means implementing administrative, physical, and technical safeguards. All three matter. And missing one can create gaps.
Step 4: Risk Monitoring & Review
Risks and controls need continuous monitoring to make sure they’re actually working. That means reviewing these on a regular basis:
- Information system activity logs
- Incident management reports
- Policy compliance
Update your risk register whenever something changes. Think:
- Material changes to policies and procedures
- Organizational restructuring
- Technology shifts
- New regulations
Step 5: Communication & Reporting
Report risk findings to leadership, board governance, and relevant regulatory bodies as required. Transparency matters at every level.
It also matters on the front lines. Build a culture where staff feel safe reporting near-misses and safety concerns without fear of punishment.
What Is Enterprise Risk Management (ERM) in Healthcare?
Most healthcare organizations manage risks in silos.
- The clinical team handles patient safety
- The legal team handles compliance
- IT handles cybersecurity
Each team works independently. And that’s a problem.
Enterprise risk management (ERM) takes a different approach. It’s a holistic, organization-wide framework that brings all risk domains together under one roof. Instead of duplicating effort across departments, ERM identifies overlapping requirements and manages them centrally.
ERM also goes beyond basic compliance. It aligns risk management with the organization’s strategic objectives. This turns risk oversight into a tool for better decision-making. As a result, the organization doesn’t treat it like a regulatory obligation.
Many ERM programs take this further with a Healthcare GRC model:
- Governance covers accountability
- Risk management covers identification and mitigation
- Compliance covers ongoing adherence
Together, they form a single connected framework.
Risk management technology makes this possible at scale. Specialized GRC platforms give leadership real-time, enterprise-wide visibility into risks across all domains (clinical, operational, financial, legal, and technology).
If your organization is considering an ERM approach, consult compliance experts experienced with customizable healthcare risk management software. The right guidance makes a significant difference.
Who Is Responsible for Risk Management in Healthcare?
Risk management isn’t the responsibility of a single person. It requires participation across the entire organization.
Key Roles
The following roles share responsibility for identifying, managing, and monitoring risks across the healthcare organization.
- Chief risk officer (CRO) / Chief compliance officer (CCO). They’re responsible for the enterprise risk management strategy. They also have to report risks to executive leadership and the board.
- Risk manager. They oversee the day-to-day management of the risk register. They also review incident tracking and mitigation planning.
- Compliance team. They ensure adherence to regulatory requirements. They also support risk assessments related to HIPAA, CMS, OSHA, and other regulations.
- Clinical leadership (CNO, CMO, nurse managers). They’re responsible for clinical and patient safety risk domains. Their role also involves implementing clinical practice guidelines.
- IT/security team (CISO, IT director). They manage technology infrastructure and cybersecurity risks. They also ensure that the organization complies with the HIPAA Security Rule.
- All staff. Every employee needs to identify and report risks. A strong risk culture requires organization-wide participation.
- Board of directors/governance. They provide oversight and ultimate accountability for the organization’s overall risk posture.
Key Risk Management Frameworks and Standards in Healthcare
You don’t have to build a risk management program from scratch. These established frameworks give you a solid foundation.
HIPAA Security Rule (45 CFR §164.308)
It requires a security management process that includes:
- Regular information system activity reviews
- A remediation plan
- A risk assessment
- A sanctions policy
Everything must be documented and retained for at least six years.
NIST Cybersecurity Framework (CSF) 2.0
This is one of the most widely adopted frameworks for managing cybersecurity risk. Healthcare organizations that use NIST CSF 2.0 experience smaller increases in cybersecurity insurance premiums.
CMS Conditions of Participation
This sets the baseline standards for hospitals and health systems participating in Medicare and Medicaid. It covers environmental and operational risk management requirements that every participating institution must meet.
ISO 31000
The ISO 31000 is an international standard. It provides principles and guidelines for enterprise risk management. It applies across industries, including healthcare.
It offers a useful structure for institutions building an ERM program.
Health Industry Cybersecurity Practices (HICP)
HICP provides sector-specific cybersecurity guidance designed for healthcare organizations.
The HIPAA Journal says that adoption is strong in email protection (86%) and cybersecurity governance (83%). However, medical device security lags behind at just 48%. That gap is worth paying attention to. This is because connected devices are becoming more common in clinical settings.
Common Challenges in Healthcare Risk Management
Even well-run organizations encounter obstacles when managing risk. Here are some of the most common challenges.
Siloed Risk Management
When different departments manage risks independently, compliance efforts get duplicated. And holistic risk visibility disappears. Nobody sees the full picture.
Reactive vs. Proactive Culture
Many healthcare organizations still respond to risks only after something goes wrong. That approach is backwards. A proactive culture identifies threats before they turn into incidents.
Legacy Systems
Outdated technology, such as EHR systems and practice management software, creates cybersecurity vulnerabilities. It also slows remediation timelines. It’s one reason healthcare organizations often lag behind in resolving vulnerabilities. Even when they identify risks right away.
Resource Constraints
Smaller practices often lack dedicated risk management staff. Compliance responsibilities fall to administrators who are already stretched thin.
You can work with one of Hello Rache’s Healthcare Virtual Assistants®. They’re HIPAA-trained and provide on-demand administrative support for audits and documentation. This offers scalable help without the overhead.
AI & Emerging Technology Risk
Healthcare organizations are still in the early stages of understanding AI-related risk. Many can identify potential concerns but are unsure how to mitigate them. That gap is continuing to grow.
Staff Training & Culture
Risk management only works if everyone participates. When staff don’t understand their role in identifying and reporting risks, even the best program breaks down.
Best Practices for Effective Risk Management in Healthcare

Effective risk management requires structured processes and consistent execution.
Adopt an Enterprise (ERM) Approach
Break down risk silos. Use one cohesive framework with unified reporting. There, integrate clinical, operational, financial, legal, and technology risks. Fragmented programs often miss important connections.
Conduct Regular, Documented Risk Assessments
Don’t treat risk assessment as a one-time checkbox. Conduct formal assessments at least once per year. And whenever there are material changes to systems, regulations, or operations.
Prioritize Third-Party Risk Management
Implement standardized vendor assessments. Move away from self-attested questionnaires and adopt standardized supplier assurance frameworks. Third-party risks are too significant to manage casually.
Invest in Purpose-Built Technology
Risk management technology and GRC platforms provide real-time visibility and automate workflows. They also keep documentation requirements on track.
Train All Staff — Not Just Compliance Teams
Provide role-specific risk assessment training when policies change. Build a safety culture where staff reports near-misses without fear of punishment. Everyone plays a part.
Align with Established Frameworks
Ground your program in recognized standards. These include HIPAA, NIST CSF, and Joint Commission guidelines. This demonstrates regulatory good faith and strengthens overall program quality.
Integrate Risk Management into Strategic Planning
Don’t treat risk management as a compliance burden. Treat it as a strategic asset. Do this by linking it to organizational goals and board-level oversight.
Consult Expert Compliance Advisors
Expert guidance is especially valuable when:
- Selecting healthcare risk management software
- Conducting HIPAA risk assessments
- Designing ERM programs
Services like Hello Rache’s virtual medical assistants provide HIPAA-compliant support for:
- Administrative tasks
- Documentation
- Audit prep
It provides you with remote assistants who are qualified nurses. The rate is $9.50 per hour. There are no setup fees. Plus, there’s no contract, and you can opt out at any time.
This frees your team to focus on high-value risk work without the overhead of full-time hires. The right expertise saves time and prevents costly mistakes.
For example, Indeed reports that the average salary for a full-time medical administrative assistant in the U.S. is nearly $ 45,000 per year.
There are also the costs per hire. These are the costs a company incurs during the recruiting process. This could be around $2,500 (or more), according to Indeed. And this could include software, advertising, and relocation expenses.
Building a Stronger Risk Culture in Healthcare
Risk management in healthcare isn’t a one-time compliance exercise. It’s an ongoing, organization-wide discipline that:
- Supports your organization’s long-term mission
- Safeguards confidential health data
- Ensures regulatory compliance
- Protects patients
The practices and frameworks covered in this guide work together. Clinical, operational, financial, legal, and technology risks are interconnected. Managing them in a coordinated way is what separates reactive organizations from resilient ones.
Healthcare organizations that invest in proactive, enterprise-wide risk management are better positioned to:
- Earn the trust of patients and partners
- Avoid costly enforcement actions
- Prevent harm
That trust is difficult to build and easy to lose.
The time to act is now. Don’t wait for an incident to happen.
Ready to strengthen your practice’s risk and compliance support?
SCHEDULE A CONSULTATION with Hello Rache today. See how our virtual assistants can help your team stay organized, compliant, and focused on patient care.
Frequently Asked Questions About Risk Management in Healthcare
What is HIPAA’s Role in Healthcare Risk Management?
HIPAA’s Security Rule (45 CFR §164.308) requires healthcare organizations to conduct a risk assessment. It should identify all threats to electronic protected health information.
Organizations must then develop an action plan. This is to remediate identified risks and document all related activities. These risk assessments are a core component of healthcare risk management programs. And it’s important to review them regularly. And ensure ongoing compliance with federal data protection requirements.
What Is Clinical Risk Management in Healthcare?
Clinical risk management focuses on risks directly tied to patient care. That includes:
- Hospital-acquired infections
- Surgical complications
- Diagnostic failures
- Medication errors
Healthcare institutions use clinical risk management programs to:
- Identify potential safety issues
- Implement preventive controls
- Improve clinical protocols
The goal is to reduce adverse events and strengthen patient safety practices. In other words, you’re improving the overall quality of care.
What Software Is Used for Risk Management in Healthcare?
Healthcare organizations use purpose-built risk management technology and GRC platforms to
- Generate compliance documentation
- Automate risk assessments
- Manage the risk register
- Track remediation
These platforms centralize risk data. They also provide leadership with visibility across clinical, operational, financial, and cybersecurity risks. The right platform makes risk management programs easier to run, track, and audit.
P.S. At Hello Rache, we prioritize HIPAA compliance and make sure that our virtual assistants follow strict data protection protocols when supporting healthcare teams with administrative workflows and documentation. If you want a deeper look at the requirements healthcare organizations must meet, read our HIPAA compliance checklist guide.






