Dental claim denials still affect roughly 10% to 15% of submissions nationwide, DSN reports. For a busy dental practice, that often means unpaid work, delayed reimbursements, and tighter cash flow. Front desk teams spend hours following up with insurance companies instead of supporting patients. If this feels familiar, you’re not alone.
So, what is dental billing? Dental billing is the process of submitting, tracking, and resolving insurance claims and patient balances so services are paid accurately and on time.
This guide explains how the process works today, where revenue commonly slips through the cracks, and how support models like Hello Rache help practices stay efficient without sacrificing the patient experience.
Highlights
- Dental billing directly impacts cash flow, claim denials, and long-term practice profitability.
- Accurate documentation, correct CDT coding, and timely claim submission are critical to getting paid on time.
- Most billing issues stem from insurance verification errors, coding mistakes, and delayed follow-up on denied claims.
- Modern tools and dental-trained virtual assistants help practices reduce administrative burden and protect revenue.
What Is Dental Billing?
At first glance, dental billing can sound like basic office work. But in reality, it touches almost every part of a dental practice. It connects patient care to payment and determines how reliably the practice gets paid.
Core Definition
Dental billing is the process a dental practice uses to submit and follow up on insurance claims with insurance companies to ensure payment for completed care. It begins once treatment is documented and continues until the insurer pays its portion and the patient has settled their balance.
This process is different from medical billing.
Medical claims depend on:
- Complex medical necessity rules
- ICD-10 diagnosis codes
- CPT codes
Dental claims rely on CDT codes. These are tied to defined benefits within dental insurance plans, not open-ended coverage.
Clinical documentation links billing codes to the actual care provided. Clinical notes and records, like periodontal charting, explain why the team used specific CDT codes. If the documentation does not clearly support the billed procedure, the claim is likely reduced or denied. Claims processing teams rely on this link to approve payment.
Key Components of Dental Billing
Every successful dental billing process follows the same core structure. These steps work together to:
- Keep payments moving
- Reduce denied claims
- Prevent errors
When even one part is missed or rushed, delays usually manifest later as rework or lost revenue.
- Patient demographic information. Correct names, birthdates, and contact details help prevent claim rejections before review.
- Insurance verification. Coverage and eligibility are confirmed before treatment to avoid payment issues later.
- Payment posting. Insurance payments and adjustments are recorded accurately in the patient account.
- CDT code application. Services are assigned the correct CDT codes recognized by insurance plans.
- Treatment documentation. Clear clinical notes explain the procedures your team has performed. And also why they were needed.
- Claim submission. Completed claims are sent to the right insurance carrier using the ADA form.
- Patient billing. Remaining balances are billed clearly once insurance has paid.
Who Handles Dental Billing?
In many offices, dental receptionists handle billing. This approach can work when claim volume is low. But as insurance rules grow more complex, billing tasks often compete with patient-facing duties, leading to staff overload.
Some practices hire in-house billing specialists or a dedicated billing coordinator to manage claims and follow-ups full-time. Others choose to outsource billing to an external company.
Hello Rache offers a flexible alternative by providing dental-trained virtual assistants who handle billing and insurance verification remotely. This allows in-office teams to stay focused on patient care.
The Dental Billing Process: Step-By-Step
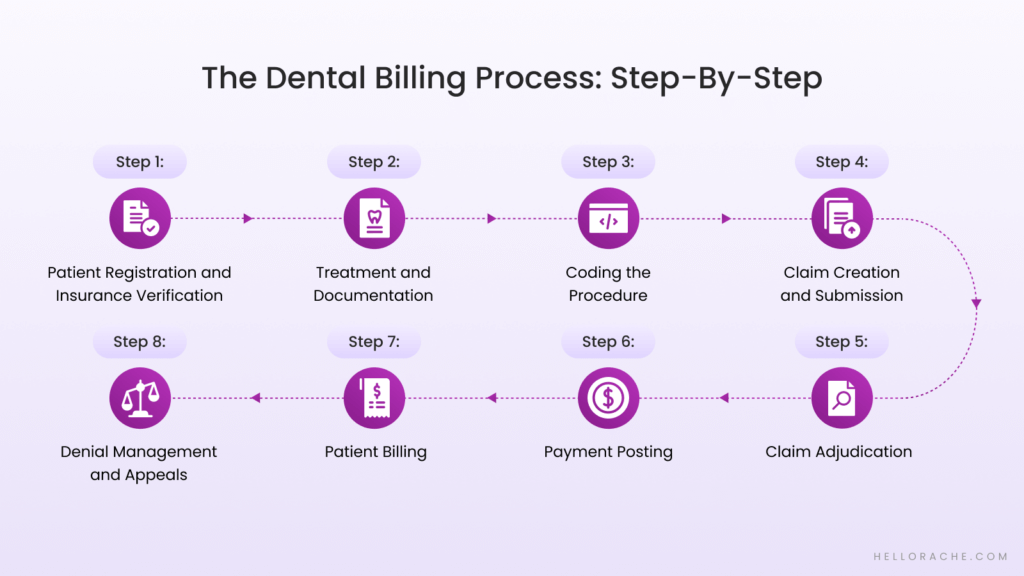
Understanding the journey of a claim is the only way to find leaks in your revenue. It is a long road from the first call to the final check. This is how it works.
Step 1: Patient Registration and Insurance Verification
Everything starts with accurate patient registration. Names, dates of birth, and insurance IDs must be correct. Even a single wrong digit can trigger an automatic rejection before a claim is ever reviewed.
Insurance verification comes next. Coverage should be confirmed for the service data, including deductibles and remaining benefits. For procedures, such as crowns, checking pre-authorization rules in advance helps prevent denials that could have been avoided.
Step 2: Treatment and Documentation
Once care begins, you have to focus on documentation. Dental hygienists and assistants must clearly document what was done and why. These notes support patient care. But they also serve as proof for insurance reviewers when a claim is questioned.
Take scaling and root planing, for example. Without detailed periodontal charting that shows active disease, insurers may deny payment. Vague notes invite pushback and raise audit risk. Clear, complete documentation protects both revenue and compliance.
Step 3: Coding the Procedure
Coding is the process of converting clinical care into a billable claim. Each service is translated into a CDT (current dental terminology) code, so insurance companies know exactly what was performed. These codes guide how the provider reviews the claim and how they calculate payment.
For example, exams, cleanings, and crowns each have specific CDT codes tied to coverage rules. Common examples include
- D1110 for cleanings
- D2740 for crowns
- D0120 for exams
Accuracy matters. Incorrect coding can lead to denials or reduced payments. More serious errors, such as upcoding or downcoding, increase audit risk and may trigger repayment issues. Staying current with CDT updates helps protect both revenue and compliance.
Step 4: Claim Creation and Submission
Once documentation and coding are complete, the claim is ready to be sent. Today, most practices submit claims electronically. This helps catch missing information or errors before the claim ever reaches the insurance company.
Timing matters as much as accuracy. Most payers expect claims to be submitted within 24 to 72 hours of treatment. Each ADA claim must include correct primary and secondary insurance details. Missed deadlines can turn valid claims into unrecoverable balances.
Step 5: Claim Adjudication
After a claim is submitted, the insurance company begins its review. The claim is checked against coverage rules, benefit limits, and provider contracts. This process can take anywhere from a few days to several weeks. This depends on the payer and the procedure’s complexity.
During review, insurers may request additional information, such as X-rays or written narratives. Afterward, the results appear in the Explanation of Benefits (EOB). The EOB outlines:
- What was paid
- What was adjusted or denied
- What the patient still owes
Step 6: Payment Posting
When payment arrives, payment posting begins. Payments and contractual adjustments are recorded in the practice management system.
This step often reveals underpayments or errors. Catching them early keeps accounts receivable accurate.
Step 7: Patient Billing
After insurance pays, any remaining balances are billed to the patient. Statements are sent, often through automated systems.
When needed, payment plans help patients manage costs and improve collections.
Step 8: Denial Management and Appeals
Even well-run billing systems see denied claims. Common causes include:
- Missing documentation
- Coverage limits
- Coding errors
What matters most is how quickly the denial is addressed. Delays allow balances to age, increasing the risk of lost revenue.
Successful appeals follow a clear process. Successful appeals follow a clear process. The issue has been identified, supporting records have been corrected, and the claim has been resubmitted promptly. Hello Rache’s trained billing specialists track denial trends across insurance carriers and help practices adjust coding and documentation. This reduces repeat denials over time.
Common Dental Billing Challenges
Running a dental office comes with a unique set of administrative headaches. Identifying these challenges is the first step toward solving them and protecting your practice revenue.
Insurance Verification Errors
Outdated or incorrect insurance details are a common cause of rejected claims. When eligibility is not checked before each visit, coverage issues surface after treatment. Consistent verification workflows help keep information current and prevent avoidable denials.
Coding Errors
Incorrect CDT codes, missing documentation, or procedures that do not match clinical notes weaken claims. Even small coding errors can lead to reduced payments or denials. Regular training and documentation reviews help ensure billing accuracy and compliance.
Claim Denials and Rejections
Dental claim denial rates remain high nationwide. Most denials stem from documentation gaps, coding errors, or coverage limits. Beyond delayed payment, denials drain staff time. Claims that are never appealed often turn into permanent revenue loss.
Time-Consuming Manual Processes
Manual data entry and insurance follow-ups slow many dental offices. This administrative burden pulls staff away from patient-facing work and adds pressure behind the scenes.
The Medical News Bulletin reports that healthcare professionals consistently cite administrative workload as a leading cause of burnout. Repetitive paperwork disrupts workflows and increases stress.
Virtual dental assistants from Hello Rache ease that strain by taking routine billing tasks off your team’s plate. This keeps workflows moving and allows in-office staff to focus on patients instead of paperwork.
Keeping up With Insurance Changes
Insurance rules change often and vary by carrier. Credentialing and network participation add complexity. Staying current requires focused attention that busy offices may struggle to maintain internally.
Patient Payment Collection
Collecting patient portions becomes harder when costs are not clearly communicated. Without written policies, payment plans, and automation, balances linger in accounts receivable. Clear expectations and structured payment options help improve collections and reduce confusion.
Best Practices for Efficient Dental Billing
To run a successful dental practice, you need more than just great clinical skills. You need an efficient administrative engine. Here are some practices that can help transform your billing process.
- Verify insurance before every appointment. Use real-time eligibility checks and standard protocols to confirm coverage and explain costs upfront.
- Implement accurate documentation habits. Complete clinical notes, periodontal charting, and radiographs should clearly support the codes used.
- Submit claims promptly. Aim for same-day or next-day submission. Submitting claims electronically helps reduce delays and missed deadlines.
- Use practice management software effectively. These include integrated billing features, automated claim scrubbing, and reporting capabilities that reduce manual effort. Hello Rache’s virtual assistants are trained across major dental software platforms.
- Stay current on CDT codes and insurance policies. Review annual CDT code updates, monitor insurance policy changes, and train your team so billing decisions are always accurate.
- Monitor accounts receivable regularly. Review aging reports, set clear benchmarks, and follow up on balances at 30, 60, and 90 days before they become uncollectible.
- Establish clear patient financial policies. Use written policies, provide upfront cost estimates, and offer flexible payment options to reduce confusion and improve collections.
- Consider outsourcing or virtual support. When billing tasks strain your team, specialized support helps. Hello Rache provides dental-trained virtual assistants who efficiently manage billing, insurance verification, and collections.
The Financial Impact of Effective Dental Billing
Effective dental billing improves revenue cycle optimization by reducing the time between care and payment. When claims are clean and follow-ups are consistent, days in accounts receivable drop. That leads to higher collection rates and fewer balances aging into write-offs. The result is steadier cash flow without increasing patient volume.
Practices also see measurable ROI. Fewer denials mean less rework and faster reimbursement. Many offices reduce costs by using virtual billing support rather than full-time staff. Compared to in-house hires, virtual assistants provide skilled billing help without benefits, overhead, or downtime. This helps improve margins while maintaining consistent billing.
How Technology Is Transforming Dental Billing
Technology has changed how medical and dental billing works behind the scenes. Today, billing is faster, more accurate, and far less manual. Many issues are identified before a claim reaches the payer. This saves time and revenue.
Here are just some of the benefits of integrating technology with dental billing:
- Electronic claims and clearinghouses move claims faster and reduce delays caused by missing data.
- AI-powered coding assistance flags coding issues early by reviewing clinical notes before submission.
- Analytics and reporting tools give real-time insight into payments, denials, and practice revenue.
- Automated insurance verification confirms coverage directly inside scheduling and billing systems.
- Patient payment portals support online billing, faster payments, and automated reminders.
Hello Rache’s tech-savvy virtual assistants are trained on modern dental platforms and help practices use these tools consistently, without adding pressure to in-office teams.
As part of their onboarding, they train using Curve Dental, a cloud-based dental software widely used in dental offices. This hands-on experience helps them understand real scheduling, insurance verification, charting, and billing workflows, so they can step into your processes smoothly and support your revenue cycle with confidence from day one.
Getting Dental Billing Right for Long-Term Practice Success
In our What is Dental Billing guide, we’ve seen that strong dental billing is essential to practice success. It takes more than sending claims. It requires knowledge, consistency, and dedicated follow-through across the entire revenue cycle. When billing is handled well, practices get paid on time, reduce denials, and create a smoother patient experience.
Now is the right time to review how your billing actually works day-to-day. Small gaps add up quickly.
Ready to streamline your dental billing process?
and discover how dental virtual assistants from Hello Rache can transform your revenue cycle and help your team stay focused on patient care.






